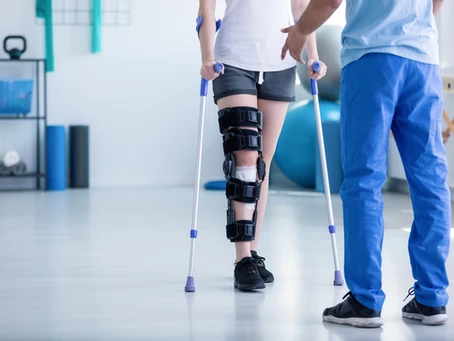
So you tried physical therapy and other conservative measures, but you found no relief. Maybe you were talked into a surgery by a silver-tongue physician who likely didn’t know better or that Physical Therapy was even a good option for you to begin with, unfortunately it happens all the time. This is one reason you should, at least, consult with a Physical Therapist for your injuries, aches and pains prior to most MD. We have specialized training in dealing with the joints; bones and muscles, plus others, and have tested higher than any other doctorate field when it comes to this outside of orthopedic surgeons.
On to why you came here – surgical precautions. This is where things can become a little confusing for patients, mostly because, 1. A lot of times from my experience, the patient is being told these precautions while they’re heavily medicated from anesthesia so memory is challenging. 2. The precautions change depending on which surgeon performed the surgery! So you go online maybe and see, hmmm, that’s very different than what I was told. Or the other one, what surgery was that? Did he call it a Mumford Procedure or was that just a Clavical Resection, are they the same? Did he call it a Clavioplasty? Do you feel like you started to make up words there and now you can’t even get ahold of anyone to get the actual name? You would ‘think’ that there’s some universal set of rules that explain, if you have done ‘XYZ’ surgery, they you have ‘XYZ’ rules to follow until ‘XYZ’ timeline and then it’s full speed ahead. The reality is there are surgeons who are still giving out hip precautions, despite no adverse events associated with ignoring them, there are rotator cuff repairs that are mild repairs, no complications or comorbidities and they have 16 weeks of sling time.
Obviously there are reasons to have longer restricted periods, but all too often I see people who are being held back, be it out of fear o surgical failure or ignorance to the body’s resilience. As someone who spends the majority of their day around people who were once broken down and defeated, but are now fully capable of whatever they want it tends to skew your thinking to the “let’s get this thing going already.” Some of my best patients with regard to outcomes and timelines to full recovery were the ones who, within reason, ignored a lot of my, and their surgeons orders with regard to use of sling/minimize activity. I would like to see more studies done in this area. We are knocking on the door right now with hip and knee replacements and getting them to out-patient physical therapy the next day now, so I imagine it’s only a matter of time.
Shoulder Surgeries – A lot of times you’re going to be in a sling and told not wo use that arm actively to raise or lift anything for 6 weeks or so on your own. You’ll be going through Physical Therapy around the end of this timeline (4-6wk) as well and begin to start adding in assisted movements and passive stretching by the therapist. You’ll be doing gripping and neck movements to maintain joint ROM, probably the most common is pendulums where you let your arm dangle and spin it/swing it using hip momentum. Unless we’re talking about reverse shoulder replacements and other select surgeries, the ultimate goal is always to maximize ROM to normal values (at least to what your other arm has) and then progressively strengthen that joint. The recovery to full use varies and will largely depend on comorbidities and mental fortitude as the stiffness and pain can sometimes be moderate-severe. Typical full use, feeling back to 100% and deep into the strengthening phase of the rehab will be 24 week/6 months.
Knee Replacements – One of my favorites to see. These surgeries are painful and a lot of my patients report wishing they would have just suffered and got both done at the same time. These used to be overnight at hospital stays and then 2 weeks of home health therapy. Now they are starting to do more next day outpatient services and are finding faster recovery and improved outcomes in the shorter terms. Knees come to us a few weeks following replacement/immediate now and we focus on range of motion again to start. There will be lighter muscle engagement exercises and other joint strengthening around the knee, like the hip and ankle, while we try to maximize ROM and decrease short term pain. You’ll be walking through this time and likely using a walker depending on upper body strength and function. If my patients aren’t at 50%-75% (Toe slightly behind knee if sitting in chair) range of motion/compared to the other knee, by the 4 week mark then I feel like I’ve let them down. By 8 weeks you aren’t going to be perfect and you’ll likely have a lot of weakness still, but you should be walking pretty well at this point and have full range. Everyone heals at their own pace and things like diabetes and other health factors can certainly slow this down. This one is tricky with full recovery, but the timelines to full use and feeling close to 100% should be close to the 6mo mark and back to life as you know it. There will be continued bone modeling for a year or two.
Ankles and Wrists – Very similar issues and make up of the peripheral limbs when you think about it. Often times both of these if fractured will get some variation of plates and screws and call it an ORIF, Open-reduction Internal-Fixation. Lots of words to say it’s held together from the inside and we had to open the arm to do it with an incision. Compare to the old school contractions of the marionet of rods and metal going through the skin, which would be an external fixation. If ankle, you’ll likely be non-weight bearing and they’ll put you in a boot with a scooter or give you crutches. Wrists will be told to protect it and given a shell/brace to wear to protect it and serve as an exoskeleton/reminder to not use for heavy door opening/loading to push yourself up or catch you to sit/fall. You’ll be doing active movements usually around the 2-3 week mark, but still unable to put weight through it. This will typically be progressed from non-weight to toe-touch weight-bearing, partial weight-bearing, full weight-bearing. For the wrists you can skip the toe-touch and just go partial to full weight-bearing. Usually based on timelines and not necessarily function due to tissue healing timelines. We can ‘facilitate’ improvements with recovery, but at the end of the day there is definitely a time component whether we want to believe it or not. Sometimes after the bones have healed nice they will go in and remove the hardware, sometimes not. If there’s no symptoms and it’s not preventing any loss of function personally I don’t see the value in risking another operation, and regress on my recovery a few weeks.
Hip Surgeries/Knee Ligament/Tendon/internal surgeries – These surgeries are a lot of times the most debilitating and humbling as they really take away a lot of our mobility and independence and force us to rely on our loved ones, if they’re able to and around. Thing like ACL tears will minimize quad function for some time which makes walking hard, even when it’s tolerable and not stiff as a board. For ACL tears and athletes being reinjured you really shouldn’t get back before 9mo, even with good functional measures. Hip microfractures can delay weight-bearing by 6-8 weeks which just prolongs the feeling of being helpless. Half of the battle, or more, in Physical Therapy is mental, if your physical therapist isn’t addressing this you need to find a new therapist. If you’re getting a Labral repair you may be non-weight bearing for a couple of weeks before gradually returning this to normal by 2 months. Progressing ROM at the same time and then entering the strengthening phase respecting symptoms and tissue healing principles.
If you’ve made it this far and had any questions, fill out our form below and we will respond to you immediately with some free resources and ways to improve your current situation at no cost to you!
At the end of the day, you have to understand that while these precautions and restrictions aren’t set in stone, they are there for your own benefit and if you had any doubts on whether you should do something or not, I would err on the side of not. If you recently have had a surgery and are feeling down in the dumps because it’s not going your way, or you feel like you’re behind someone you know who had the same one, let’s setup a FREE Discovery Visit to see what’s going on and help to provide some information for your specific case. We want to help you.